Introduction to Medical Cannabis and the Endocannabinoid System

The History of Cannabis
Written sources document the cultivation and use of the plant dating back at least to the third millennium B.C., and possibly even to the pre-ceramic Neolithic period (ca. 8800–6500 B.C.). Cannabis was used for fiber, food, and for medicinal, religious, and recreational purposes. Evidence of this can be found in Neolithic artifacts as well as in ancient China and India; the Scythians and Hindu saints also used the plant. In the 19th century, its medical use gained prominence in the West. The 20th century saw widespread restrictions worldwide, before more recent trends toward decriminalization emerged—a reflection of the long and evolving history of this plant.
Source: Dr. Russo, E.B., “History of Cannabis and Its Preparations in Saga, Science, and Sobriquet,” 2007.

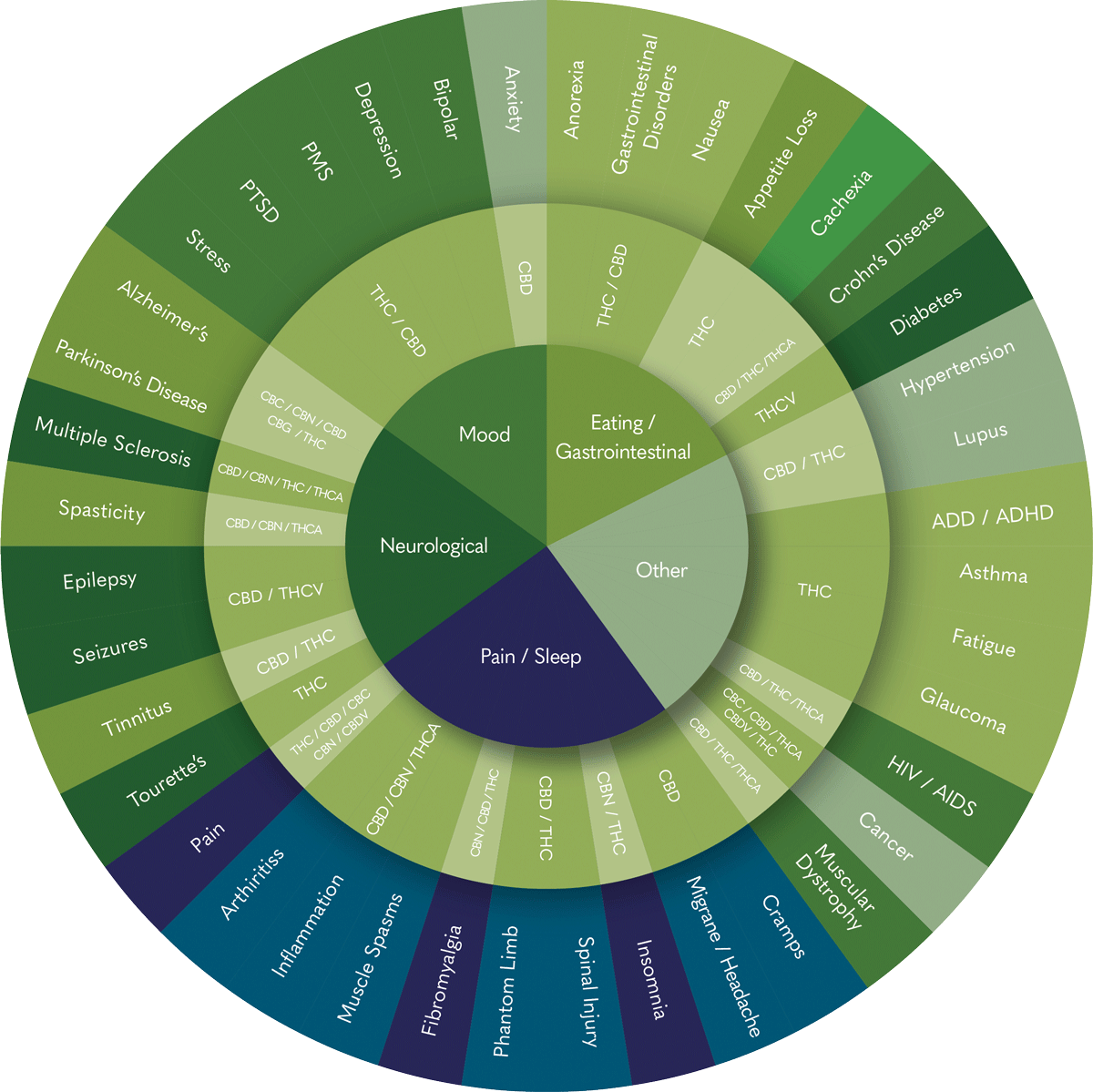
Common medical applications
Phytocannabinoids act on the endocannabinoid system (ECS). For this reason, medical research is investigating their potential for treating various conditions. Data from the German BfArM companion survey (2022) as well as international reviews show that this has led to several medical applications:
-
Chronic pain, arthritis, inflammation, muscle spasms, fibromyalgia, phantom pain, spinal cord injuries, insomnia, migraines, and other headaches.
-
Alzheimer's disease, Parkinson's disease, multiple sclerosis, spasticity, epilepsy, seizures, tinnitus, and Tourette syndrome.
-
Anxiety, bipolar disorder, depression, PMS, PTSD, and stress.
-
Anorexia (significantly reduced food intake), gastrointestinal disorders, nausea, loss of appetite, cachexia, Crohn's disease, and diabetes.
-
High blood pressure, lupus, ADD/ADHD, asthma, fatigue (severe exhaustion), glaucoma, HIV/AIDS, cancer, and muscular dystrophy.
Sources: BfArM,“Final Report on the Accompanying Study,” 2022); Health Canada, “Information for Health Care Professionals,” 2018); NASEM,“The Health Effects of Cannabis and Cannabinoids,” 2017).

Under what conditions is medical cannabis prescribed?
Therapeutic goals and potential benefits
Medical cannabis is primarily considered for severe, chronic conditions when standard treatments have been exhausted or are not well tolerated. This approach is based, among other things, on the current DGS clinical practice guidelines (2024) and data from the BfArM’s accompanying survey. The focus is on the following clinical objectives:

Managing chronic pain:
Especially neuropathic (nerve-related) pain.
The goal is a significant reduction in pain intensity (“pain relief”) rather than complete freedom from pain. By influencing pain perception in the central nervous system, patients often report an improved ability to cope with persistent symptoms.

Effects on spastic symptoms:
Multiple sclerosis (MS) and other neurological disorders.
Clinical studies have reported effects on muscle stiffness and spastic symptoms under certain conditions.

Symptom management in palliative care:
Oncology and severe chronic diseases.
It is described as part of supportive therapy to manage the side effects of intensive treatments.

Improving quality of life:
Side effects of chronic conditions.
A key benefit identified in accompanying German studies is an improvement in sleep quality and overall well-being.
Sources:
DGS Clinical Practice Guidelines,“Clinical Practice Guideline: Cannabis-Based Medications in Pain Medicine (Version 2.0)” 2024
BfArM, “Final Report on the Monitoring Study Conducted Pursuant to Section 31(6) of Book V of the Social Code on the Prescription and Use of Cannabis Medicines,” 2022. (Download Link)
The Endocannabinoid System (ECS)
The endocannabinoid system (ECS) is a widespread signaling system in the human body and plays a role in regulating numerous physiological processes. One of its key functions is maintaining homeostasis—that is, the body’s dynamic internal balance.
The system consists of three core components:
Endocannabinoids—the body’s own neurotransmitters:
Lipid-based signaling molecules produced by the body itself. Among the most extensively studied are anandamide (AEA) and 2-arachidonoylglycerol (2-AG).Receptors (CB1 and CB2):
G protein-coupled receptors found in the central and peripheral nervous systems, in immune cells, and in various other tissues.Enzymes: Enzymatic synthesis and degradation pathways regulate the concentration, intensity, and duration of endocannabinoid signaling.

CB1 receptors are found throughout the body, but are primarily located in the brain. Their role is to facilitate communication within the nervous system.
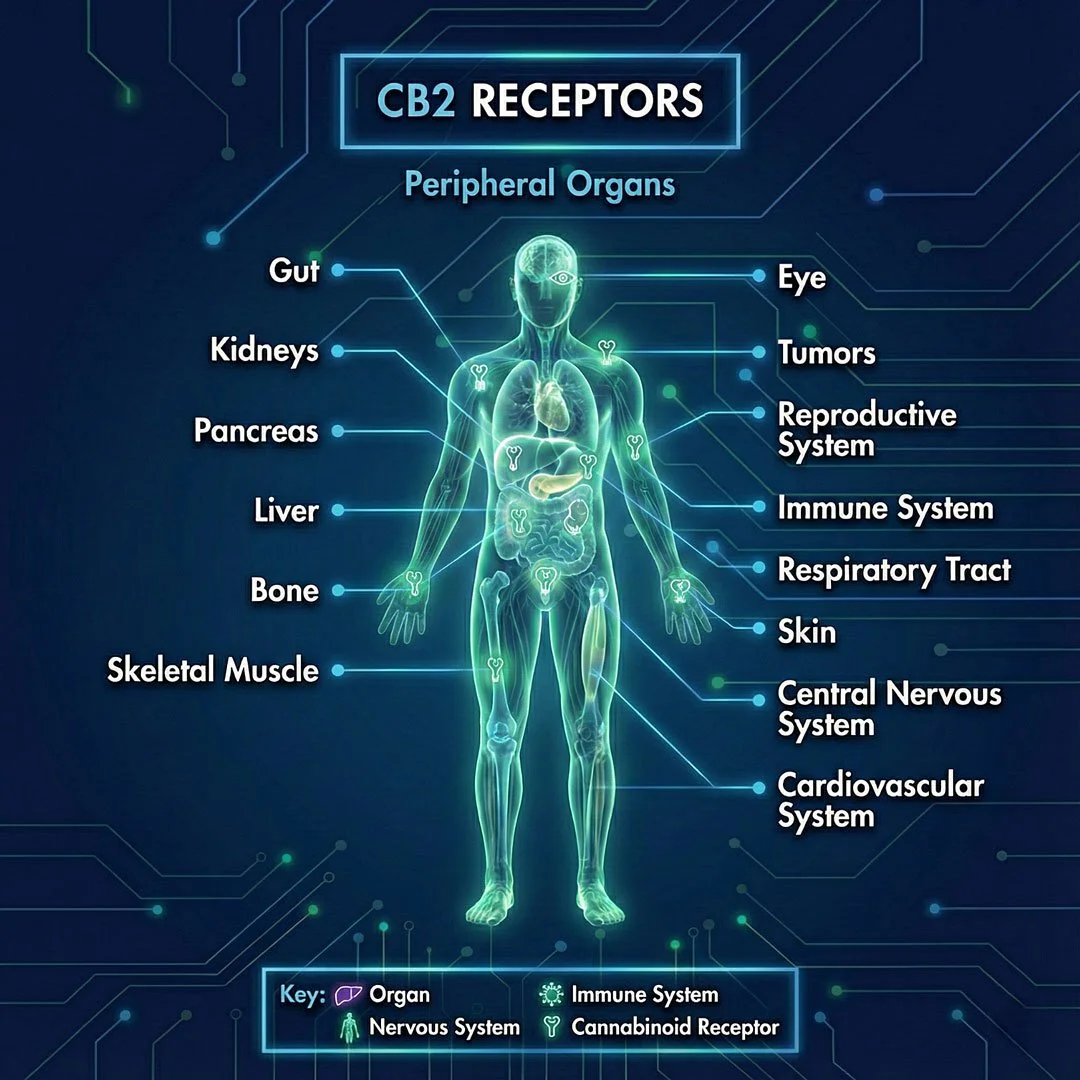
CB2 receptors are distributed throughout the body. They specifically regulate communication between the organs and the immune system.
Here’s how it works: A classic “lock-and-key” analogy provides a clear explanation of the endocannabinoid system. Cannabinoid receptors can be thought of as “locks” on the cell surface, while endocannabinoids act as “keys” that bind specifically to these receptors and initiate intracellular signaling processes.
In situations such as pain, inflammation, or stress, endocannabinoid signaling contributes to the adaptive regulation of physiological processes. The endocannabinoid system does not function as a binary on/off mechanism, but rather enables context-dependent fine-tuning and stabilization of homeostasis
Source: Pertwee RG (Ed.). Handbook of Cannabis. Oxford University Press, 2014.
What do cannabinoid receptors (CB1 and CB2) do?

Phytocannabinoids – plant-based active compounds with biological significance
The cannabis plant produces over 100 bioactive compounds known as phytocannabinoids .
Some of these plant compounds share structural and functional similarities with the body’s own endocannabinoids, allowing them to interact with and modulate the endocannabinoid system (ECS).
THC (Δ9-tetrahydrocannabinol) (
):
THC is the primary psychoactive phytocannabinoid in the cannabis plant. In a medical context, THC is used for its effects on the central nervous system, including muscle relaxation, modulation of pain perception, and appetite stimulation.
CBD (cannabidiol):
CBD is a non-psychoactive phytocannabinoid.
It is being extensively studied for its modulatory effects on inflammatory signaling pathways, stress-related processes, and muscle tone, without producing the intoxicating effects typical of THC.
The "entourage effect" (phytocomplexity)
In addition to THC and CBD, medical cannabis contains numerous other classes of compounds, such as terpenes (aromatic, sometimes biologically active components) and flavonoids.
The concept commonly referred to as the “entourage effect”describes the hypothesis that various plant compounds interact pharmacodynamically with one another and can thereby modulate overall efficacy and tolerability.
Although this model remains a subject of scientific debate, it is frequently cited to explain the differences between full-spectrum products and isolated individual compounds.

How is the treatment prescribed?
(Rx). This means that a strict “last-resort” requirement is no longer a formal prerequisite for prescribing in every case.
However, specific requirements and a prior approval process still apply for coverage by statutory health insurance (GKV).
Use this 4-step overview to prepare specifically for your medical consultation.
Phase One: Preparing the Documents
Even though cannabis is no longer subject to the Narcotics Act (BtMG), a clear medical justification is still required for a prescription. Structured documentation supports a medically sound decision.
Compiling the “Treatment History”
To document your health status in a clear and comprehensive manner, please consider the following points:
List of diagnoses: Relevant medically documented diagnoses and findings that support the indication (e.g., chronic pain syndrome, multiple sclerosis, migraine).
Current status: A brief description of your symptoms and how they affect your daily life.
Previous Treatments: An overview of the pharmacological and non-pharmacological therapies used to date, including documented efficacy, side effects, and reasons for discontinuing treatment.
Why this is helpful: Even though structured documentation is not strictly required for a private prescription, it helps the treating physician make a well-founded assessment of the medical appropriateness and proportionality of a treatment in each individual case.
Phase Two: The Consultation
Patients do not need a “cannabis specialist,” but rather a doctor who is willing to consider treatment with cannabis-based medications as part of an individualized treatment plan.
The consultation during the medical appointment
Who can prescribe it:
Any licensed physician in Germany—with the exception of dentists and veterinarians—may prescribe medical cannabis provided there is a medical indication.The current legal framework:
Medical cannabis does not have to be prescribed only after all other treatment options have been exhausted. The key factor is that, in the individual case, a serious illness is present and a generally accepted standard treatment is not available, is not suitable, or has not been sufficiently effective.Here’s how to broach the subject: You can approach the conversation in a factual and open manner, for example: “I’m interested in treatment options that focus on symptom relief and good tolerability. Given the current legal framework, could treatment with medical cannabis be medically appropriate in my case?”

Phase Three: The Reimbursement Request
If you want statutory health insurance (GKV) to cover the costs of treatment with cannabis-based medications, you must submit a formal application for coverage. This application must be submitted jointly by you and your treating physician.
The role of the treating practice: The treating practice prepares the medical justification. This document outlines the indication, the severity of the condition, and the reasons why treatment with cannabis-based medicines is medically indicated.
The insured person’s role: You submit the request for coverage along with all the necessary documents to your health insurance provider.
Evaluation criteria: In order for costs to be covered under Section 31(6) of the German Social Code, Book V (SGB V), it is generally required that a serious illness be present and that a generally accepted treatment in line with medical standards is either not available, cannot be applied in the specific case, or is not expected to yield sufficient therapeutic success.
Timeline: Once a complete application has been submitted, statutory health insurance providers are required to make a decision within three weeks.
Phase Four: Cost Coverage and Prescription Processing
Once your prescription has been filled, it can generally be filled at any pharmacy.
Redeem your prescription
Where can the prescription be filled: Prescriptions for medical cannabis can generally be filled at any German pharmacy. However, since not every pharmacy stocks cannabis-based medications, it may be necessary to place an order in some cases.
Availability and Ordering: If the prescribed product is not immediately available, the pharmacy can usually obtain it through an authorized wholesaler. Delivery times may vary depending on product availability and shipping logistics.
Advice at the pharmacy: Pharmacists will provide you with information on proper use, the dosage prescribed by your doctor, and practical matters such as storage and handling.



Important Legal Notice for Patients
The content provided on this website is for general informational purposes only. It does not constitute medical advice and is not a substitute for consulting a licensed physician or other qualified healthcare professional.
This website does not promote self-diagnosis or self-medication. Decisions regarding medical treatments—including the prescription of cannabis-based medications—are made exclusively by licensed medical professionals based on an individual medical assessment.
Medical cannabis is subject to national regulations and may only be prescribed for appropriate medical indications and in accordance with applicable legal provisions.
We strive to keep the information on this website accurate and up-to-date. However, medical knowledge and legal frameworks may change over time.
For further information and the sources used, please see References & Further Reading .











